Endoscopic Spine Surgery vs Traditional Spine Surgery: Which One Is Safer?
Medicine Made Simple Summary
Spine surgery is sometimes needed when problems such as a slipped disc or nerve compression cause severe pain or weakness that does not improve with medication or physiotherapy. Traditional spine surgery involves making a larger incision to access the spine and remove the tissue pressing on nerves. Endoscopic spine surgery is a newer minimally invasive technique where surgeons use a thin tube with a camera to treat the problem through a very small incision. Both procedures aim to relieve nerve pressure and reduce pain, but they differ in surgical approach, recovery time, and impact on surrounding muscles and tissues.
Understanding Why Spine Surgery Is Sometimes Needed
Back pain is extremely common, and most people experience it at some point in their lives. In many cases, the pain improves with rest, medication, physiotherapy, or lifestyle changes.
However, some spine conditions can cause persistent nerve compression that does not respond to conservative treatments. When this happens, surgery may be recommended to relieve pressure on the affected nerve.
Conditions such as herniated discs, spinal stenosis, or nerve root compression can cause symptoms like severe back pain, sciatica, numbness, tingling, or muscle weakness.
The goal of spine surgery is to remove the source of nerve pressure and restore normal nerve function. Over time, surgical techniques have evolved to become more precise and less invasive.
Two commonly discussed approaches today are traditional spine surgery and endoscopic spine surgery, and patients often research endoscopic spine surgery patient experience to understand what the treatment journey may involve.
Suggested Image: Diagram showing spinal nerve compression caused by a herniated disc.
What Is Traditional Spine Surgery?
Traditional spine surgery, often referred to as open spine surgery, has been used for many decades to treat spinal conditions.
In this approach, surgeons make a larger incision in the back to reach the affected part of the spine. The muscles surrounding the spine are gently moved aside to allow access to the vertebrae and discs.
Once the surgeon reaches the problem area, the portion of the disc or bone that is pressing on the nerve is removed.
This procedure can effectively relieve nerve pressure and reduce pain. In some cases, additional procedures such as spinal fusion may be performed to stabilize the spine.
Traditional spine surgery remains an important treatment option for certain complex spine conditions.
Suggested Image: Illustration showing open spine surgery with a larger incision.
What Is Endoscopic Spine Surgery?
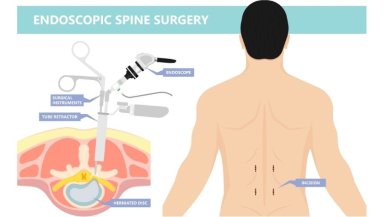
Endoscopic spine surgery is a minimally invasive technique designed to treat certain spine problems using much smaller incisions and is often explained in detail when discussing the endoscopic spine surgery procedure.
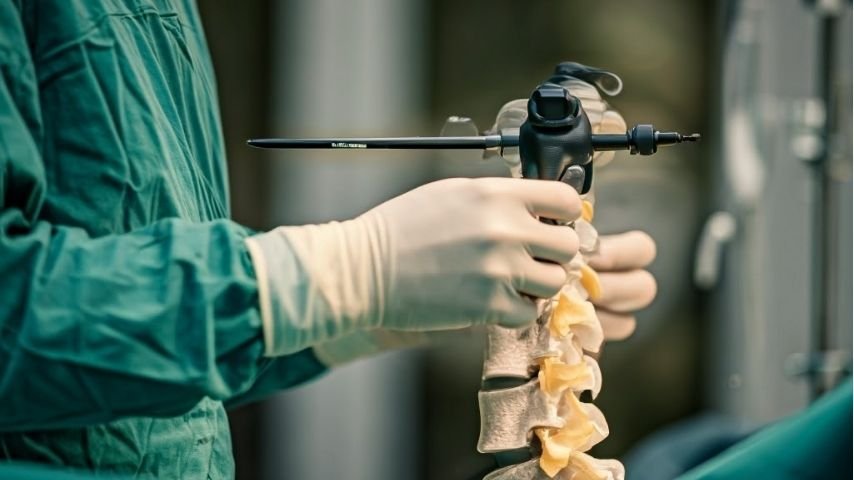
In this procedure, surgeons use a thin tube called an endoscope that contains a camera and light source. The camera allows the surgeon to view the spine on a monitor in high detail.
The endoscope is inserted through a small incision in the skin, usually less than one centimeter in size.
Through this tube, surgeons insert specialized instruments to remove the disc material or tissue pressing on the nerve.
Because the procedure requires minimal disruption of muscles and surrounding tissues, patients often experience less postoperative pain and faster recovery.
Suggested Image: Diagram showing endoscope used in minimally invasive spine surgery.
Key Differences Between the Two Approaches
One of the biggest differences between traditional and endoscopic spine surgery is the size of the incision.
Traditional surgery usually requires a larger incision so that surgeons can access the spine directly. Endoscopic surgery uses a much smaller incision through which specialized instruments are inserted.
Another difference involves muscle disruption. Traditional surgery may require muscles to be moved aside to reach the spine. In endoscopic surgery, muscles are often preserved because the instruments pass through natural tissue pathways.
These differences can influence recovery time and postoperative discomfort.
However, both procedures aim to achieve the same goal, which is relieving pressure on the spinal nerves.
Suggested Image: Comparison diagram showing incision size differences between open and endoscopic surgery.
Recovery After Traditional Spine Surgery
Recovery after traditional spine surgery can vary depending on the type of procedure performed.
Because the incision is larger and muscles may be affected during surgery, patients may experience more postoperative discomfort.
Hospital stays may last several days depending on the complexity of the surgery.
Patients usually need several weeks or months to fully recover and return to normal activities.
Physiotherapy and rehabilitation programs often play an important role in helping patients regain strength and mobility.
Although recovery may take longer, traditional surgery can be highly effective for many spine conditions.
Recovery After Endoscopic Spine Surgery
Endoscopic spine surgery is designed to reduce tissue disruption and allow faster recovery.
Because the incision is small and muscles are minimally affected, patients often experience less postoperative pain.
Many patients are able to walk within hours after the procedure. In some cases, patients may go home on the same day or the next day.
Recovery time is generally shorter compared with traditional surgery, and many individuals return to daily activities within a few weeks.
However, recovery speed can still vary depending on the patient’s overall health and the severity of the spine condition.
Suggested Image: Illustration showing patient walking shortly after minimally invasive spine surgery.
Is Endoscopic Spine Surgery Safer?
Many patients wonder whether endoscopic spine surgery is safer than traditional surgery.
Both procedures are considered safe when performed by experienced surgeons.
Endoscopic surgery offers certain advantages because it causes less damage to muscles and surrounding tissues. This can reduce the risk of complications such as infection or excessive blood loss.
The smaller incision also usually results in less scarring.
However, endoscopic surgery is not suitable for every spine condition. Some complex cases still require traditional open surgery to achieve the best results.
The safest option depends on the specific diagnosis, the severity of the condition, and the patient’s overall health.
How Doctors Decide Which Surgery Is Best
Choosing the right surgical approach requires careful evaluation by a spine specialist.
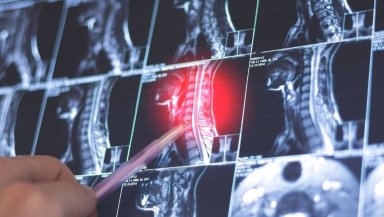
Doctors review the patient’s symptoms, physical examination findings, and imaging results such as MRI scans.
These scans show exactly where the nerve compression is occurring and help doctors determine whether minimally invasive techniques can address the problem effectively.
In many cases involving slipped discs or certain types of nerve compression, endoscopic spine surgery may be recommended, and patients often ask about endoscopic spine surgery cost and success before making a decision.
For more complex conditions such as severe spinal deformities or extensive spinal damage, traditional surgery may still be the best option.
Suggested Image: MRI scan highlighting nerve compression in the spine.
Advantages of Minimally Invasive Spine Surgery
Minimally invasive techniques such as endoscopic spine surgery offer several potential benefits for suitable patients.
The smaller incision typically results in less muscle damage and reduced postoperative pain.
Patients may experience shorter hospital stays and faster return to daily activities.
Reduced blood loss during surgery is another advantage.
However, the effectiveness of the procedure depends on proper patient selection and surgical expertise.
Not every patient with back pain requires surgery, and doctors carefully evaluate each case before recommending treatment.
The Importance of Early Diagnosis and Treatment
Persistent back pain or nerve symptoms should not be ignored.
Early diagnosis allows doctors to determine the cause of the problem and recommend appropriate treatment.
Many spine conditions can be managed successfully with non-surgical methods when detected early.
If surgery becomes necessary, minimally invasive techniques may provide effective relief while minimizing recovery time.
Understanding the available treatment options helps patients make informed decisions about their care.
Conclusion
If you are experiencing persistent back pain, sciatica, or nerve-related symptoms that do not improve with conservative treatment, consulting a spine specialist can help identify the cause. A detailed evaluation can determine whether minimally invasive procedures such as endoscopic spine surgery or other treatments may help relieve nerve compression and restore comfortable movement.