The operation is performed under anaesthesia. You may feel a little soreness near the incision after surgery. It usually eases within a few days and improves with the tablets' pain relief.

- Introduction
- What Is Endoscopic Spine Surgery?
- Why Is Endoscopic Spine Surgery Done?
- Right Candidate for Endoscopic Spine Surgery
- Who May Not Be Suitable for Endoscopic Spine Surgery?
- Endoscopic Spine Surgery Procedure
- During the Procedure
- After Endoscopic Spine Surgery
- Risks and Complications of Endoscopic Spine Surgery
- Benefits of Endoscopic Spine Surgery
- Why Choose Gleneagles Hospitals for Endoscopic Spine Surgery?
- Conclusion
Introduction
Neck and lower back pain are frequently managed without surgery. In many individuals, symptoms settle with medication and physiotherapy, along with modifications in daily activity.
In some patients, nerve compression does not settle with initial treatment. Ongoing pressure can produce radiating limb pain, numbness, or weakness. When these symptoms continue, surgical management may be explored. One minimally invasive option is endoscopic spine surgery, which allows access to the affected level through a small incision under camera guidance. Suitability for this method is determined only after careful clinical and imaging evaluation. Let’s understand it in detail.
What Is Endoscopic Spine Surgery?
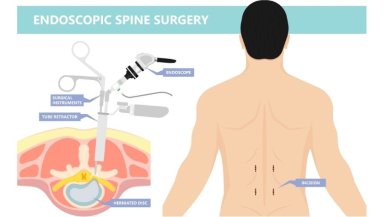
Endoscopic spine surgery uses a small camera system introduced through a narrow tube. The surgeon views the operative field on a screen during the procedure.
Specialised instruments are passed through the same channel to remove the tissue causing nerve compression. Most commonly, this involves removing part of a herniated disc. In some cases, small portions of bone or ligament are trimmed to create additional space for the nerve.
This method may be considered in:
Lumbar disc prolapse
Cervical disc herniation
Foraminal stenosis
Selected spinal canal narrowing
Certain recurrent disc cases
Because the incision is small and muscle disruption is limited, recovery patterns may differ from conventional open procedures.
Why Is Endoscopic Spine Surgery Done?
Surgical management may be considered in patients with documented nerve compression who continue to experience symptoms despite adequate conservative treatment. It is generally not advised for back pain without signs of nerve compression.
Doctors may suggest this procedure when:
Radiating arm or leg pain follows a typical nerve distribution
A disc prolapse seen on MRI corresponds with clinical findings
Ongoing numbness or weakness affects function
Reduced walking tolerance is linked to nerve compression
Symptoms recur after earlier disc intervention
A clear correlation between examination findings and imaging is required before proceeding with surgery. At Gleneagles Hospitals, treatment decisions are made after detailed clinical assessment and review of imaging studies.
Right Candidate for Endoscopic Spine Surgery
The endoscopic technique is not appropriate in every spinal condition. Suitability varies according to the level involved and the nature of the problem.
Patients who may be evaluated include:
Those with a single-level disc herniation
Individuals whose symptoms correspond with MRI findings
Patients who have completed non-surgical treatment without relief
People experiencing persistent radicular pain
Selected cases of foraminal narrowing suitable for targeted decompression
A detailed spine assessment helps determine whether this approach is appropriate.
Your health matters – get expert advice today.
Who May Not Be Suitable for Endoscopic Spine Surgery?
In some situations, another surgical strategy may be more suitable. Endoscopic surgery may not be recommended in patients who:
Have spinal instability requiring stabilisation
Show marked spinal deformity
Have extensive central canal narrowing
Have an active infection of the spine
Are medically unfit for anaesthesia
Alternative options are discussed when necessary.
Endoscopic Spine Surgery Procedure
Endoscopic spine surgery is performed by a spine surgeon trained in minimally invasive techniques. At Gleneagles Hospitals, the procedure takes place in an operating theatre equipped for spine surgery and continuous monitoring.
Before the operation, imaging studies are reviewed carefully. The surgical plan, expected outcomes, and potential risks are discussed with the patient. A review of medical history and current medications is undertaken as part of preoperative planning. Baseline blood investigations are performed prior to surgery.
Patients are commonly advised to:
Food and fluids are avoided for several hours before surgery
Any blood-thinning medicines should be discussed with the treating doctor
Help at home during the first few days of recovery should be arranged
At Gleneagles Hospitals, patients are counselled about postoperative care and discharge before the procedure.
During the Procedure
Anaesthesia is administered in accordance with the surgical requirements.
A limited skin incision is created at the identified spinal level. Imaging is used to guide the placement of the working channel. The endoscope then allows direct viewing of the affected nerve.
The compressive disc material or tissue is removed carefully under visual control. After confirming decompression, the instruments are withdrawn, and the incision is closed in layers.
The duration differs between cases. Cardiovascular and respiratory parameters are observed continuously.
After Endoscopic Spine Surgery
Once surgery is completed, patients remain in the recovery room while the team observes their condition. In many cases, assisted mobilisation begins the same day, depending on comfort and neurological status.
Some effects noted after surgery may include:
Mild soreness at the incision site
A feeling of stiffness during early movement
Occasional tingling that gradually settles
The duration of hospital stay is not uniform. Discharge may take place the same day in some cases, while others remain overnight for observation. Follow-up visits are arranged to assess healing and symptom improvement.
Risks and Complications of Endoscopic Spine Surgery
Although minimally invasive, endoscopic spine surgery carries recognised surgical risks. Complications are uncommon when appropriate selection and technique are applied.
Possible complications include:
Infection
Bleeding
Temporary nerve irritation
Dural tear with cerebrospinal fluid leakage
Recurrent disc prolapse
At Gleneagles Hospitals, postoperative monitoring continues to ensure any concerns are addressed promptly.
Benefits of Endoscopic Spine Surgery
This technique is used to relieve pressure on affected nerves while limiting disturbance to surrounding tissues. Possible benefits include:
A smaller skin incision
Less muscle handling during surgery
Reduced postoperative discomfort in appropriate cases
Shorter duration of hospital stay
Quicker return to routine activities
Its use depends on whether the expected benefit matches the patient’s specific spinal condition.
Why Choose Gleneagles Hospitals for Endoscopic Spine Surgery?
Endoscopic spine surgery is part of Gleneagles Hospital's spine care services. The program involves spine surgeons trained in minimally invasive methods, with anaesthesia and perioperative support teams.
Facilities available include:
Spine-designated operating theatres
Imaging assistance during surgery
Postoperative observation facilities
Guidance for rehabilitation after discharge
At Gleneagles Hospitals, patients are assessed before surgery and continue under follow-up care as clinically required.
Conclusion
Endoscopic spine surgery is sometimes advised when a compressed nerve continues to cause discomfort, tingling, or weakness even after a reasonable trial of non-surgical treatment. Many patients first try medicines, rest, guided exercises, or injections. If these measures do not bring sufficient relief, a surgical option may then be discussed.
At Gleneagles, doctors carry out a detailed assessment. The dedicated spine team reviews the patient’s symptoms, examines them carefully, studies scan findings, and considers any existing medical conditions. Surgery is recommended only when these factors together suggest that the patient is likely to benefit from this technique. You can visit us and speak with our medical professionals if you have any queries.
Dr Naveen M A
HOD & Sr Consultant - Minimal Access Brain and Spine Surgery
MBBS, MS, MCh (Neuro), FMAS, FMISS (Seoul), FASS (USA), Fellow Skull base Endoscopy (USA)
Frequently Asked Questions
Recovery is different for each individual. You may gradually return to your usual activities as you feel able. Your doctor will advise you further at your follow-up visit.
Mobilisation often begins on the same day, depending on recovery and neurological status.
Some patients return home the same day. Others may remain overnight for observation.
Recurrence of disc herniation is possible in a small percentage of cases. Follow-up and adherence to medical advice help reduce this risk.