Risks and Complications of Endoscopic Spine Surgery: What Your Surgeon Will Explain Before Surgery
Medicine Made Simple Summary
Endoscopic spine surgery is a minimally invasive procedure used to treat spine conditions such as slipped discs and sciatica. In this surgery, doctors use a thin tube with a small camera called an endoscope to reach the affected area of the spine through a very small incision. The surgeon removes the portion of the disc or tissue that is pressing on the nerve. This helps relieve pain, numbness, and weakness caused by nerve compression. Although the procedure is generally safe and recovery is usually faster than traditional surgery, like any medical procedure it carries certain risks that patients should understand before surgery.
Why It Is Important to Understand Surgical Risks
When patients are advised to undergo spine surgery, they often focus on the benefits of the procedure. Relief from severe pain, improved mobility, and the ability to return to normal activities are important goals of treatment.
However, it is equally important to understand the possible risks and complications associated with any surgical procedure. Knowing these risks helps patients make informed decisions and prepares them for the recovery process.
Endoscopic spine surgery is considered a safe and effective procedure when performed by experienced surgeons. Because it uses a minimally invasive approach, many risks associated with traditional open surgery are reduced, which is why many patients research endoscopic spine surgery vs traditional spine surgery when considering treatment options.
Even so, doctors always explain potential complications so that patients can fully understand the procedure and know what to expect.
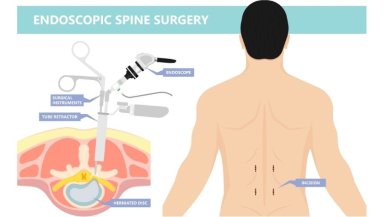
Suggested Image: Illustration showing endoscopic instrument inserted through a small incision in the spine.
Understanding How Endoscopic Spine Surgery Works
Endoscopic spine surgery uses specialized equipment that allows surgeons to treat spine problems through very small openings in the skin.
During the procedure, a small incision is made near the affected part of the spine. A thin tube containing a tiny camera is inserted through this incision.
The camera sends images to a monitor, allowing the surgeon to clearly see the structures inside the spine.
Using small surgical instruments inserted through the tube, the surgeon removes the portion of the disc or tissue that is pressing on a nerve.
Once the pressure on the nerve is relieved, the instruments are removed and the small incision is closed.
Because the surrounding muscles and tissues are minimally disturbed, patients usually experience less pain and faster recovery compared with traditional surgery, which contributes to a positive endoscopic spine surgery patient experience.
Common Risks Associated With Spine Surgery
Although endoscopic spine surgery is minimally invasive, it still involves operating near delicate structures such as nerves and the spinal cord.
For this reason, surgeons carefully evaluate each patient before recommending the procedure.
Most complications are uncommon, but understanding them helps patients recognize symptoms that may require medical attention.
Complications can occur during surgery, immediately after surgery, or during the recovery period.
Fortunately, modern surgical techniques and careful monitoring have significantly reduced the risk of serious complications.
Infection
Infection is a potential risk associated with any surgical procedure.
Although the incision used in endoscopic spine surgery is very small, bacteria can occasionally enter the surgical site.
Symptoms of infection may include redness, swelling, warmth around the incision, fever, or increased pain.
Doctors take several precautions to reduce the risk of infection. Surgical instruments are sterilized, and antibiotics may be given before or after the procedure.
Most infections, if they occur, can be treated effectively when detected early.
Suggested Image: Illustration showing surgical wound care and healing.
Bleeding
Bleeding during surgery is another possible complication.
Because endoscopic spine surgery involves a small incision and minimal tissue disruption, blood loss is usually much lower compared with traditional open surgery.
However, minor bleeding may still occur during the procedure.
Surgeons use specialized instruments and techniques to control bleeding and ensure clear visibility during surgery.
Significant bleeding is uncommon but may require additional medical attention if it occurs.
Nerve Irritation or Injury
The spine contains many nerves that control movement and sensation in different parts of the body.
During spine surgery, surgeons work very carefully around these nerves to relieve pressure without causing damage.
In rare cases, nerves may become irritated or injured during the procedure.
This may lead to temporary symptoms such as numbness, tingling, or weakness.
Permanent nerve injury is extremely rare but is one of the reasons why spine surgery should always be performed by experienced specialists.
Suggested Image: Diagram showing spinal nerves and nerve root compression.
Persistent or Recurring Symptoms
Some patients may continue to experience symptoms even after surgery.
This may happen if the nerve has been compressed for a long time before treatment. In such cases, the nerve may take time to heal.
Occasionally, a disc herniation may occur again in the future. This is known as recurrence.
Maintaining good posture, following rehabilitation exercises, and avoiding heavy strain on the spine can help reduce the risk of recurrence.
Doctors monitor patients during follow-up visits to ensure that recovery is progressing well.
Reaction to Anesthesia
Endoscopic spine surgery usually requires anesthesia so that the patient remains comfortable during the procedure.
Although anesthesia is generally safe, some patients may experience mild reactions such as nausea, dizziness, or temporary confusion after surgery.
Anesthesiologists carefully evaluate the patient’s medical history before surgery to minimize these risks.
Monitoring during and after surgery ensures that any reactions are managed quickly.
Blood Clots
After any surgery, there is a small risk of developing blood clots in the legs.
These clots can form if blood circulation slows during prolonged periods of inactivity.
Doctors encourage early walking and movement after surgery to help maintain healthy circulation and support faster endoscopic spine surgery recovery time.
Compression stockings or other preventive measures may also be used to reduce the risk.
Suggested Image: Illustration showing patient walking after surgery to improve circulation.
How Doctors Minimize Surgical Risks
Modern surgical techniques and careful planning have greatly improved the safety of spine surgery.
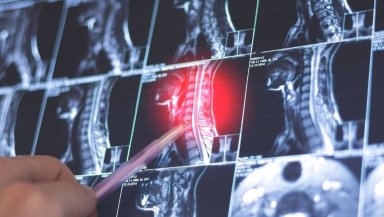
Before recommending endoscopic spine surgery, doctors conduct detailed evaluations including physical examinations and imaging tests such as MRI scans.
These tests help identify the exact location of the problem and determine whether minimally invasive surgery is appropriate.
During surgery, advanced imaging and high-definition cameras allow surgeons to operate with great precision.
After surgery, patients are monitored closely to ensure that recovery progresses safely.
The Importance of Following Post-Surgery Instructions
Patients also play an important role in preventing complications after surgery.
Following the doctor’s instructions regarding wound care, medications, and physical activity helps promote proper healing.
Avoiding heavy lifting, sudden twisting movements, and strenuous activities during recovery protects the spine.
Participating in recommended physiotherapy programs can strengthen the muscles supporting the spine and reduce the risk of future problems.
Regular follow-up appointments allow doctors to monitor healing and address any concerns.
Suggested Image: Illustration showing physiotherapy exercises for spine recovery.
Understanding That Most Patients Recover Well
Although the possibility of complications can seem concerning, it is important to remember that most patients recover well after endoscopic spine surgery.
The minimally invasive nature of the procedure often leads to less postoperative pain and faster return to normal activities.
Advances in medical technology and surgical training continue to improve outcomes for patients undergoing spine procedures.
By understanding the potential risks and working closely with their healthcare team, patients can approach surgery with confidence and realistic expectations.
Conclusion
If you are experiencing persistent back pain, sciatica, or symptoms of nerve compression, consulting a spine specialist can help determine whether minimally invasive procedures such as endoscopic spine surgery may be appropriate. A thorough evaluation allows doctors to explain both the benefits and potential risks so that you can make an informed decision about your treatment.
References and Sources
American Association of Neurological Surgeons