Why Is My Distal Pancreatectomy Recovery So Slow? Common Reasons and What’s Normal
Medicine Made Simple
Distal pancreatectomy is a major surgery where the body and tail of the pancreas are removed, and sometimes the spleen is also removed. Many patients expect to feel better quickly after surgery, but recovery often feels slower than expected. Tiredness, pain, poor appetite, digestion problems, drain discomfort, and emotional stress are all common during healing. Internal recovery takes much longer than the skin wound healing. Slow recovery does not always mean something is wrong. Understanding what is normal after surgery helps reduce fear, improves patience, and helps patients know when medical attention is truly needed.
What Is a Distal Pancreatectomy?
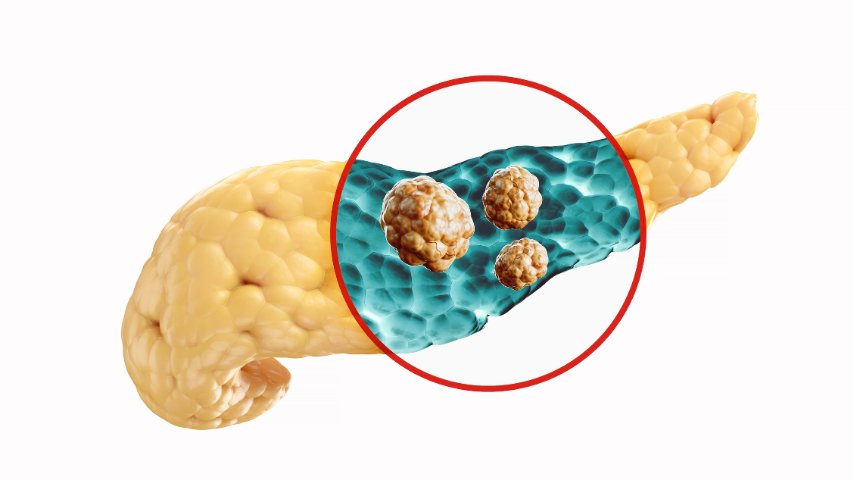
A distal pancreatectomy is a surgery where the body and tail of the pancreas are removed. This operation is commonly done for pancreatic tumors, cysts, chronic pancreatitis, neuroendocrine tumors, or pancreatic cancer affecting the left side of the pancreas, and EUS for pancreatic disorders.
The pancreas is an important organ that helps in two major ways. It produces digestive enzymes that help break down food, and it also produces hormones like insulin that help control blood sugar levels. When part of the pancreas becomes diseased, surgery may be needed to remove that affected portion while protecting the rest of the body.
Since the spleen sits very close to the tail of the pancreas, it is often removed during the same surgery. This is called distal pancreatectomy with splenectomy. The surgery may be done through open surgery with a larger cut or through laparoscopic vs open distal pancreatectomy laparoscopic or robotic surgery using smaller cuts. Even when smaller cuts are used, it is still a major operation and recovery takes time.
Why Recovery Feels Much Slower Than Expected
Many patients feel frustrated because they expect recovery to be faster. Once the surgery is completed, they often assume healing should happen quickly, especially if the skin wound looks small or neat from the outside.
But pancreatic surgery is not only about the visible incision. The body is healing internally from the removal of part of an important organ, inflammation caused by surgery, changes in digestion, pain, reduced movement, and sometimes the removal of the spleen as well.
Patients are often recovering from:
- Internal tissue healing
- Digestion changes
- Pain and weakness
- Reduced mobility
- Emotional stress related to diagnosis
- Blood sugar changes
This is why many patients say they feel confused and disappointed when recovery feels slow. The outside wound may look better, but inside the body, healing is still happening. That is completely normal and expected.
Fatigue: The Most Common Complaint
One of the most common complaints after distal pancreatectomy is extreme tiredness. Many patients say the fatigue feels worse than the pain itself. Even simple tasks like taking a shower, walking to the kitchen, or climbing stairs may feel exhausting.
This happens because surgery places a major stress on the body. Healing requires a large amount of energy. The body is working hard even when the patient is resting. Poor appetite, weight loss, pain medicines, low blood count after surgery, poor sleep, and emotional stress can all make fatigue worse.
Patients may also feel mentally tired. Worrying about test results, future treatment, and slow recovery adds emotional exhaustion to physical weakness. It is very common for fatigue to last several weeks and sometimes even longer.
Recovery usually improves slowly, not suddenly. Patients should not expect to wake up one day and feel completely normal.
Pain That Lasts Longer Than Expected
Many people worry when pain continues after leaving the hospital. They assume that once they are discharged, pain should be almost gone. This is not always true.
Pain after distal pancreatectomy may include discomfort around the incision, deeper abdominal pain, drain site pain, bloating, gas pain, and sometimes shoulder pain after laparoscopic surgery. Some patients also develop back discomfort because movement is reduced during recovery.
Pain usually improves slowly over time. Some days feel better, and some days feel worse, especially after increased activity. This does not automatically mean something is wrong.
However, severe new pain, rapidly worsening pain, or pain that comes with fever should always be checked by a doctor. The goal is not to ignore pain, but to understand which pain is part of normal healing and which pain needs medical attention.
Poor Appetite and Digestion Problems
Many patients become worried because eating feels difficult after surgery. This is one of the biggest reasons recovery feels slow and frustrating.
Patients often experience:
- Feeling full very quickly
- Bloating
- Nausea
- Loose stools or constipation
- Greasy stools
- Discomfort after fatty foods
- Unwanted weight loss
The pancreas helps digest food, especially fats. When part of it is removed, digestion may temporarily change. The body also needs time to recover after anesthesia and abdominal surgery.
Small frequent meals usually work much better than large meals. Soft foods and simple home-cooked meals are often easier to tolerate during the first few weeks. Some patients may need pancreatic enzyme tablets to help digestion and improve food absorption.
Poor appetite is common, but if eating becomes very difficult or weight loss becomes severe, medical review is important.
Surgical Drains Can Make Recovery Feel Worse
Many patients go home with a surgical drain still in place, and this often creates anxiety. Patients usually feel that they cannot truly recover until the drain is removed.
The drain is used to remove extra fluid and help doctors monitor healing, especially to check for pancreatic leaks. While useful, it can make recovery feel uncomfortable and stressful.
Patients often experience:
- Discomfort while moving
- Trouble sleeping
- Fear of pulling the drain accidentally
- Anxiety about drain fluid
- Delayed feeling of normal recovery
Sometimes drains stay in longer than expected if fluid output remains high. This does not always mean something is seriously wrong. It often means the body simply needs more time to heal safely.
Pancreatic Leak: A Common Concern
One of the most discussed complications after distal pancreatectomy is a pancreatic leak. This happens when digestive fluid leaks from the cut surface of the pancreas after surgery.
Because the pancreas produces strong digestive enzymes, leakage can slow healing and increase the risk of infection. This is one reason doctors monitor drain output very carefully after surgery.
Possible warning signs include:
- Fever
- Increasing abdominal pain
- High drain output
- Foul-smelling drain fluid
- Delayed recovery
- Feeling suddenly worse instead of better
Not every patient with a drain has a pancreatic leak, but it is something doctors always watch closely. Most leaks can be managed well when detected early, which is why follow-up and communication with the surgical team are so important.
Blood Sugar Changes After Surgery
Another reason recovery feels slow is blood sugar instability. Since the pancreas produces insulin, removing part of it may affect blood sugar control.
Some patients notice increased thirst, frequent urination, unusual tiredness, blurred vision, or high blood sugar during follow-up testing. These symptoms can be stressful, especially for patients who never had diabetes before surgery.
Not everyone develops diabetes after distal pancreatectomy. Some people only need temporary monitoring, while others may need tablets or insulin treatment. The risk depends on how much pancreas was removed and how healthy the remaining pancreas is.
Doctors usually monitor blood sugar closely during follow-up visits. This part of recovery can feel worrying, but it is manageable with the right guidance.
Recovery Is Slower If the Spleen Was Removed
If the spleen is also removed, recovery includes additional health precautions. The spleen helps protect the body from certain serious infections, so patients without a spleen need extra awareness.
This often includes:
- Vaccinations
- Quick treatment for fever
- Stronger infection awareness
- Long-term medical precautions
Patients sometimes feel overwhelmed by this extra information after surgery. That feeling is completely understandable. Learning how to stay safe after spleen removal becomes part of long-term recovery.
Emotional Recovery Is Often Ignored
Physical healing is only one part of recovery. Many patients struggle emotionally after distal pancreatectomy, especially if the surgery was done for cancer or a suspicious tumor.
Patients may feel afraid of pathology results, anxious about future chemotherapy, frustrated with slow healing, and worried about their long-term health. Some feel stressed about finances, work, or being dependent on family members for basic tasks.
Common emotional challenges include:
- Fear about future treatment
- Anxiety about cancer diagnosis
- Loss of independence
- Frustration with slow healing
- Worry about recurrence
- Mental exhaustion
Patients often feel guilty for feeling emotional because surgery was successful. But emotional recovery is just as real as physical recovery. These feelings are normal and deserve attention.
Comparing Your Recovery to Others Creates Stress
One of the biggest mistakes patients make is comparing their recovery with someone else’s story. They hear that another person returned to work quickly or felt normal after only a short time, and they begin to worry.
Recovery depends on many factors, including age, type of surgery, open versus laparoscopic approach, presence of complications, nutrition status, diabetes, cancer treatment needs, and general health before surgery.
Slow recovery does not automatically mean bad recovery. Every patient heals differently, and comparing recovery often creates unnecessary stress and disappointment.
When Slow Recovery Is Still Normal
It is usually normal if you still have tiredness, mild pain around the incision, poor appetite, digestion changes, reduced strength, and emotional ups and downs during the first few weeks after surgery.
Many patients expect normal life to return quickly, but pancreatic surgery recovery usually takes several weeks and sometimes even months. Patients often feel discouraged because they look fine from the outside but still feel weak inside.
Patience becomes part of treatment. Healing after this type of surgery is slow because the body is doing important work that cannot be rushed.
When You Should Call Your Doctor
Some symptoms should never be ignored. While slow recovery is often normal, certain warning signs may suggest infection, pancreatic leak, or another complication.
You should contact your doctor urgently if you have:
- Fever
- Severe worsening pain
- Vomiting that does not stop
- Redness or pus from the wound
- Sudden swelling
- Chest pain
- Shortness of breath
- Very high drain output
- Foul-smelling drain fluid
- Yellowing of the eyes
- Severe weakness that suddenly worsens
Early treatment prevents bigger problems and improves recovery outcomes.
Follow-Up Visits Are Part of Recovery
Some patients think recovery ends when they leave the hospital, but this is not true. Follow-up visits are an important part of healing.
Doctors use these visits to check wound healing, remove drains if needed, monitor blood sugar, review final pathology results, assess nutrition, and decide whether more treatment such as chemotherapy is needed.
Skipping follow-up appointments can delay important treatment decisions. Recovery continues long after hospital discharge, and these visits help guide the next stage safely.
Conclusion
If your distal pancreatectomy recovery feels slower than expected, do not assume something is wrong immediately. This surgery takes time to heal, and tiredness, poor appetite, pain, and emotional ups and downs are all common parts of recovery.
The most important step is knowing what is normal and recognizing when medical help is needed. Stay connected with your surgical team, attend follow-up visits, and ask questions without hesitation.
Healing is often slower than patients expect, but with the right support, recovery becomes safer, easier, and far less frightening.
References and Sources
Memorial Sloan Kettering Cancer Center – About Your Distal Pancreatectomy
Cancer Research UK – Recovery After Pancreatic Surgery
Leeds Teaching Hospitals NHS – Distal Pancreatectomy
Baylor College of Medicine – Distal Pancreatectomy and Splenectomy