Free Flap Donor Site Explained: What It Means for Your Body and Healing
Medicine Made Simple Summary
Microvascular free flap reconstruction rebuilds damaged body parts using healthy tissue taken from another area of the same person’s body. The moved tissue carries tiny blood vessels that are reconnected under a microscope to keep it alive in its new location. The area where this tissue is taken from is called the donor site. Both the donor site and the reconstructed site heal after surgery as part of Microvascular Free Flap Recovery. Understanding donor site healing helps patients prepare for recovery and regain normal body function safely.
Introduction
When people hear they need microvascular free flap reconstruction, most of their attention goes to the body part being rebuilt. Very few think about the place where the tissue will be taken from. This area is called the donor site. Patients often say they wish they had understood donor site healing better before surgery. This guide explains donor sites in simple language so patients and families know what to expect and how the body recovers, including available Free Flap Reconstruction Options.
What Is a Donor Site in Free Flap Surgery
In free flap reconstruction, surgeons move healthy tissue from one part of the body to repair another. The place where this tissue is taken from is called the donor site. The tissue may include skin, fat, muscle, or even bone depending on what needs to be rebuilt.
Because the tissue is moved with its blood vessels, surgeons carefully separate it and then reconnect those vessels at the new location. Once moved, the donor site is closed and allowed to heal like any other surgical wound.
Understanding that there are two surgical areas helps patients prepare better. One area is being rebuilt. The other is giving tissue to help that reconstruction happen, which requires proper Free Flap Surgery Preparation.
Suggested image: Diagram showing donor site and reconstruction site on the body.
Common Donor Site Locations
Surgeons choose donor sites that provide the right type of tissue while causing the least long-term impact. Common donor areas include the thigh, lower leg, abdomen, forearm, or back. If bone is needed, part of the leg bone may be used. If soft tissue is needed, areas with extra skin and fat are chosen.
The choice depends on the reconstruction goal, body type, medical condition, and surgeon’s experience. Patients are usually examined and scans may be done to plan the safest donor site.
Every person’s body is different, so donor site selection is customized.
Suggested image: Illustration showing common donor site locations.
Why the Donor Site Matters
Many patients worry only about the reconstructed area. But donor site healing affects comfort, movement, and recovery time. Understanding donor site effects helps set realistic expectations.
The body can function normally even after tissue removal because surgeons take only what is safe to remove. Over time, surrounding muscles and tissues adjust. Most patients return to normal daily activities after healing.
Knowing that the donor site is planned carefully for safety helps reduce fear before surgery.
What the Donor Site Looks Like After Surgery
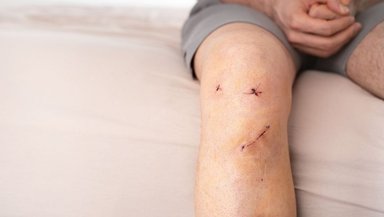
After surgery, the donor site will have stitches or staples and a dressing. There may be swelling, bruising, or soreness. This is normal. Drains may be placed temporarily to remove extra fluid.
Over the next few weeks, swelling reduces and the wound closes. A scar remains, but it usually softens and fades with time. Doctors advise how to care for the wound and when stitches will be removed.
Seeing the donor site for the first time can feel emotional. Being prepared for this makes it easier to accept the healing process.
Suggested image: Healing timeline graphic from surgery day to healed scar.
Pain and Discomfort at the Donor Site
Patients often ask if the donor site will be painful. Some soreness or tightness is expected in the early days. Pain medicines are given to keep patients comfortable. As healing progresses, discomfort reduces.
Certain donor sites may feel stiff at first, especially the thigh or leg. Gentle movement and physiotherapy help restore flexibility. Most patients report that donor site discomfort improves steadily over a few weeks.
Understanding that early soreness is temporary helps patients stay positive during recovery.
Movement and Strength After Donor Site Healing
Another common concern is whether the donor site will affect strength or movement. Surgeons plan donor sites to avoid major functional loss. In most cases, the body adapts well.
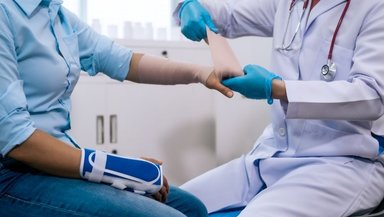
For leg or thigh donor sites, walking may feel slow at first. Physiotherapy helps rebuild strength. For forearm donor sites, hand and wrist movement are checked carefully during planning to avoid long-term problems.
With proper rehabilitation, most patients return to normal daily activities and work routines after healing.
Suggested image: Patient doing physiotherapy exercises after surgery.
Donor Site Scar and Appearance
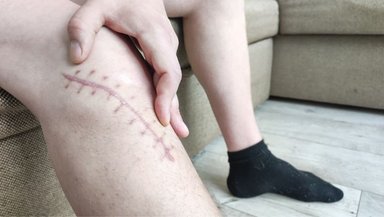
Scars are a natural part of any surgery. Donor site scars are usually placed in areas that can be covered by clothing. Over time, scars fade and become less noticeable.
Doctors may recommend scar care creams or silicone sheets to improve healing. Sun protection also helps scars fade better.
Understanding that scars improve with time prevents unnecessary worry in the early months.
How Long Does Donor Site Healing Take
Initial wound healing usually happens in two to three weeks. Full internal healing and strength recovery may take several months. The exact timeline depends on the donor site location, overall health, and whether physiotherapy is needed.
Patients are advised when to return to work, exercise, and travel. Following medical advice helps avoid complications and ensures smooth recovery.
Patience is important. Healing happens gradually, not overnight.
Possible Donor Site Complications
Most donor sites heal well, but like any surgery, there can be risks. These include infection, delayed wound healing, fluid collection, numbness, or scar thickening. Rarely, weakness may last longer than expected.
Doctors monitor donor sites during follow-up visits. Early reporting of unusual pain, redness, or discharge helps treat problems quickly.
Knowing possible risks helps patients stay alert without feeling fearful.
Emotional Feelings About the Donor Site
Some patients feel emotional about having a surgical scar in another part of the body. This is normal. Body image changes take time to accept. Support from family, counseling, or patient groups can help.
Over time, many patients say the donor site scar becomes a reminder of healing and survival. Emotional healing is just as important as physical healing.
How to Prepare for Donor Site Recovery
Before surgery, doctors may advise improving nutrition, stopping smoking, and doing gentle exercises to strengthen muscles. These steps improve healing after surgery.
Understanding which part of the body will be the donor site before surgery allows mental preparation. Asking the surgeon to show where the incision will be can reduce surprises later.
Preparation makes recovery smoother.
Why Surgeon Experience Matters for Donor Site Safety
Experienced reconstructive microsurgeons plan donor sites carefully to minimize functional and cosmetic impact. Choosing a specialized center improves the chances of smooth donor site healing.
Patients should feel comfortable asking surgeons about donor site choice, expected scars, and recovery time. Open discussion builds trust.
Suggested image: Surgeon explaining donor site plan to patient.
Life After Donor Site Healing
Once healing is complete, most patients resume normal life. Walking, working, exercising, and social activities return gradually. Donor site scars become less noticeable. Strength and flexibility improve with time.
Patients often say that understanding donor site healing beforehand made the recovery journey less stressful. Awareness replaces fear with confidence.
Conclusion
If you or your loved one is planning microvascular free flap reconstruction, ask your surgeon to explain the donor site plan in detail. Understanding where tissue will be taken from and how it will heal helps you prepare better for recovery. Schedule a consultation with a reconstructive microsurgery specialist to discuss donor site options and healing expectations.
References and Sources
American Society of Plastic Surgeons – Microsurgical Free Flap Reconstruction
Johns Hopkins Medicine – Reconstructive Microsurgery
British Association of Plastic, Reconstructive and Aesthetic Surgeons
National Cancer Institute – Reconstructive Surgery After Cancer Treatment
Memorial Sloan Kettering Cancer Center – Reconstructive Surgery Patient Guides