What Happens During Bronchoscopic Tracheal Stent Placement? A Step-by-Step Patient Guide
Medicine Made Simple
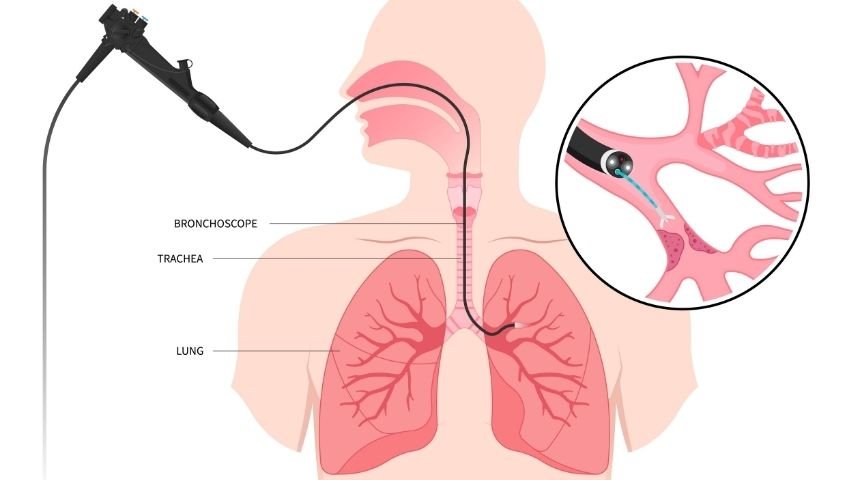
Bronchoscopic tracheal stent placement is a procedure used to open a narrowed or blocked airway so that a person can breathe more easily. Doctors place a small tube called a stent inside the windpipe using a bronchoscope, which is a thin camera inserted through the mouth or nose. The stent expands and keeps the airway open, allowing air to flow freely into the lungs. The procedure does not require large surgical cuts and is usually completed within a short time. Understanding each step of the procedure helps patients and families feel more confident and prepared for treatment, especially in cases of tracheal stenosis.
Why This Procedure May Be Needed
Breathing becomes difficult when the airway that carries air to the lungs becomes narrow or blocked. The windpipe, also known as the trachea, is the main airway that transports air from the throat to the lungs. It is supported by strong cartilage rings that help keep it open during breathing.
When the trachea becomes narrow, airflow is restricted. Even a small narrowing can cause noticeable breathing problems because airflow resistance increases as the airway becomes tighter.
Several conditions can cause this narrowing. Scar tissue may form in the airway after prolonged intubation in the intensive care unit, leading to post intubation tracheal stenosis. Tumors may grow inside the airway or press on it from nearby structures. Infections or inflammation can cause swelling that reduces the airway diameter. In some people, weakness in the airway walls causes the airway to collapse during breathing.
When these conditions significantly affect breathing and other treatments cannot maintain an open airway, doctors may recommend a tracheal stent placement.
Understanding Bronchoscopy
Bronchoscopy is a medical procedure that allows doctors to examine and treat the airways without making surgical incisions. During bronchoscopy, a thin flexible tube equipped with a camera and light is inserted through the mouth or nose and guided into the airway.
The camera sends images to a monitor so that doctors can clearly see the inside of the trachea and bronchi. This allows them to identify areas where the airway is narrow, blocked, or damaged.
Bronchoscopy is not only used for diagnosis but also for treatment. Through the bronchoscope, doctors can perform procedures such as balloon dilatation for tracheal stenosis, tissue removal, or stent placement.
This minimally invasive approach makes it possible to treat airway problems while avoiding major surgery.
Preparing for the Procedure
Before bronchoscopic tracheal stent placement, doctors perform several evaluations to understand the patient’s condition.
Imaging tests such as CT scans are often used to visualize the airway and determine the location and severity of the blockage. These images help doctors plan where the stent should be placed.
Doctors also review the patient’s medical history, medications, and any previous airway procedures. Patients are typically asked not to eat or drink for several hours before the procedure to reduce the risk of complications during sedation.
The procedure usually takes place in a specialized bronchoscopy suite or operating room equipped with advanced airway equipment.
Patients receive sedation or general anesthesia so that they remain comfortable during the treatment.
Step 1: Inserting the Bronchoscope
Once the patient is sedated, the doctor gently inserts the bronchoscope through the mouth or nose and guides it into the airway.
The camera on the bronchoscope provides a clear view of the trachea and bronchi. Doctors carefully examine the airway to locate the narrowed or blocked segment.
This step allows the doctor to confirm the exact position where the stent will be placed.
The bronchoscope also helps ensure that the airway is safe for the procedure.
Step 2: Preparing the Airway
In some cases, the airway may need to be prepared before the stent is placed. For example, if scar tissue or a tumor is partially blocking the airway, doctors may remove or reduce this tissue using bronchoscopic techniques.
Procedures such as tracheal balloon dilatation procedure may be used to widen the airway temporarily.
Preparing the airway helps create enough space for the stent and improves the effectiveness of the treatment.
Step 3: Delivering the Stent
Once the airway is ready, the doctor introduces a special delivery device that carries the stent. This device is guided through the bronchoscope to the narrowed portion of the airway.
The doctor carefully positions the stent so that it covers the entire area of narrowing. Precise positioning is important to ensure that the stent provides adequate support to the airway.
The bronchoscope camera allows the doctor to monitor the stent’s placement in real time.
Step 4: Expanding the Stent
After the stent is positioned correctly, it is released from the delivery system.
Many airway stents are designed to expand automatically once they are released. As the stent expands, it presses gently against the airway walls and holds them open.
This expansion creates a stable passage for air to flow through the airway.
The doctor then checks the stent’s position to confirm that it is properly placed and that the airway is open.
Step 5: Final Airway Inspection
Before completing the procedure, the doctor carefully inspects the airway using the bronchoscope.
This inspection ensures that the stent is stable and that there are no immediate complications such as bleeding or airway obstruction.
Once the doctor confirms that the stent is functioning properly, the bronchoscope is slowly removed.
The patient is then transferred to a recovery area where medical staff monitor breathing and vital signs.
What Happens After the Procedure
After bronchoscopic tracheal stent placement, patients are observed for a period of time to ensure that breathing remains stable.
Because sedation or anesthesia is used during the procedure, patients may feel drowsy for a few hours. Mild throat irritation or coughing may occur temporarily after bronchoscopy.
Many patients notice improvement in breathing soon after the stent is placed. Activities that previously caused breathlessness may become easier as airflow improves.
Most patients can return home the same day or after a short hospital stay, depending on their condition.
Recovery and Follow-Up Care
Recovery from bronchoscopic stent placement is usually quicker than recovery from open surgery.
Doctors schedule follow-up visits to monitor how well the stent is functioning and to ensure that the airway remains open. Imaging tests or repeat bronchoscopy may be performed if needed.
Patients are encouraged to report symptoms such as worsening breathlessness, persistent coughing, or excessive mucus production.
Regular monitoring helps detect potential issues early and ensures that the stent continues to function effectively.
Benefits of Bronchoscopic Stent Placement
One of the major advantages of bronchoscopic stent placement is that it is minimally invasive. Because the procedure does not involve large surgical incisions, recovery is generally faster and complications are less common.
The procedure can quickly restore airflow in patients with severe airway narrowing. Many patients experience noticeable improvement in breathing soon after treatment.
Bronchoscopic techniques also allow doctors to adjust or remove the stent if necessary, making the treatment flexible and adaptable to the patient’s condition.
Conclusion
Bronchoscopic tracheal stent placement is an effective treatment for severe airway narrowing caused by conditions such as tracheal stenosis, tumors, or airway collapse.
Using bronchoscopy, doctors can place a small support tube inside the airway without performing major surgery. The stent expands and holds the airway open, allowing air to move freely into the lungs.
Understanding the steps involved in the procedure helps patients and families feel more prepared and confident when doctors recommend this treatment.
With modern bronchoscopic techniques and specialized airway care, many patients experience significant improvement in breathing and quality of life.
If you or a loved one are experiencing persistent breathlessness, noisy breathing, or symptoms of airway obstruction, consult a pulmonologist or interventional pulmonology specialist. Early evaluation can determine whether treatments such as bronchoscopic tracheal stent placement may help restore comfortable breathing.
References and Sources
Cleveland Clinic – Airway Stents and Bronchoscopy

























