Bronchoscopic Tracheal Stent Placement Explained: How Doctors Open a Blocked Airway
Medicine Made Simple
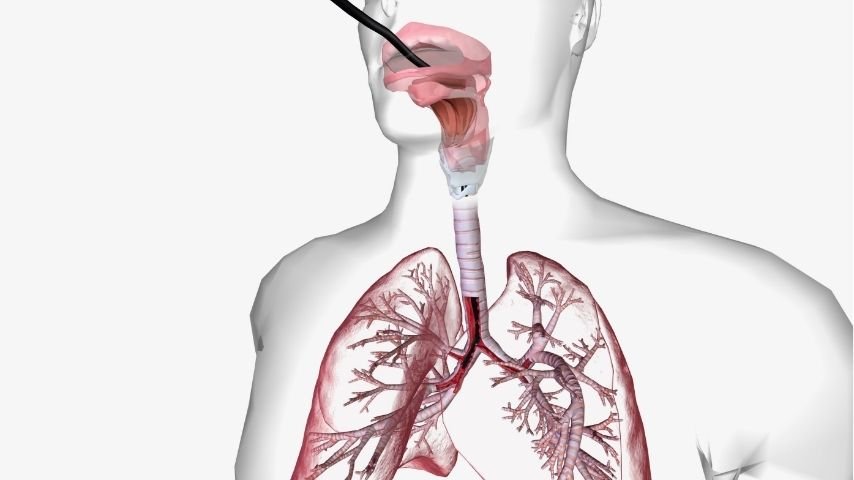
When the windpipe or large airways become severely narrowed or blocked, breathing can become difficult and sometimes life-threatening. In such cases, doctors may place a tracheal stent to reopen the airway and restore airflow to the lungs. This procedure is performed using bronchoscopy, a minimally invasive technique in which a thin camera is inserted through the mouth or nose into the airway. The stent acts like a small support tube that keeps the airway open. Bronchoscopic tracheal stent placement often improves breathing quickly and helps patients regain comfort in everyday activities.
Why Airway Blockage Can Make Breathing Difficult
Breathing depends on a clear passage between the outside air and the lungs. Air enters through the nose or mouth and travels through the throat before reaching the windpipe, also known as the trachea. The trachea then divides into two main tubes called bronchi, which carry air into the lungs.
These airways are supported by cartilage rings that help maintain their shape and keep them open during breathing. This structure allows air to move smoothly in and out of the lungs.
When the airway becomes narrow or blocked, airflow is restricted. The lungs may still be healthy, but the air cannot reach them easily. As a result, the body must work harder to breathe.
Patients with airway blockage symptoms often experience breathlessness, coughing, and noisy breathing. In severe cases, the airway obstruction may significantly interfere with normal breathing and daily activities.
When other treatments cannot keep the airway open, doctors may recommend placing a tracheal stent.
What a Tracheal Stent Is
A tracheal stent is a small hollow tube that is placed inside the windpipe to keep it open. The stent supports the airway walls and prevents them from collapsing or narrowing further.
Once the stent is positioned inside the airway, it expands and presses gently against the airway walls. This expansion creates a stable passage through which air can flow freely.
The stent acts like a structural support that keeps the airway open even if the surrounding tissue is swollen, scarred, or compressed.
By restoring airflow, the stent helps relieve breathing difficulty and improves oxygen delivery to the lungs.
When Doctors Recommend Tracheal Stent Placement
Doctors usually recommend airway stents when other treatments cannot maintain an open airway.
One common reason for stent placement is severe tracheal stenosis, a condition where scar tissue narrows the windpipe. This narrowing may occur after prolonged intubation in the intensive care unit, where a breathing tube remains inside the airway for an extended period.
Tumors that grow inside the airway or press on it from nearby structures can also block airflow. In such cases, placing a stent can reopen the airway and improve breathing.
Some patients develop airway collapse due to weakness of the airway walls, a condition called tracheobronchomalacia. A stent can provide structural support and prevent the airway from collapsing during breathing.
Infections or inflammatory conditions may also cause airway swelling that restricts airflow. If the narrowing becomes severe, a stent may be needed to maintain airway patency.
Understanding Bronchoscopy
Bronchoscopy for airway narrowing is a procedure that allows doctors to examine and treat the airways without making surgical incisions.
During bronchoscopy, a thin flexible tube with a camera and light is inserted through the mouth or nose and guided into the airway. This instrument, known as a bronchoscope, allows doctors to see the inside of the trachea and bronchi on a monitor.
Bronchoscopy provides detailed visualization of airway structures and helps doctors identify blockages, narrowing, tumors, or inflammation.
In addition to diagnosis, bronchoscopy allows doctors to perform treatments inside the airway. These treatments may include removing blockages, widening narrowed airways, or placing stents.
Preparing for Tracheal Stent Placement
Before the procedure, doctors evaluate the patient carefully to understand the nature of the airway blockage.
Imaging tests such as CT scans help visualize the airway and determine the location and severity of the obstruction. These scans provide important information that helps doctors plan the procedure.
Doctors also review the patient’s medical history and current medications. Patients are usually asked not to eat or drink for several hours before the procedure.
The procedure is typically performed in a bronchoscopy suite or operating room equipped with specialized airway equipment.
Patients receive sedation or general anesthesia so that they remain comfortable during the treatment.
Step-by-Step Overview of the Procedure
Once the patient is comfortably sedated, the bronchoscope is gently inserted through the mouth or nose and advanced into the airway.
The doctor examines the airway using the camera to identify the narrowed or blocked segment. After locating the problem area, the doctor prepares to position the stent.
A delivery system carrying the stent is passed through the bronchoscope to the affected section of the airway. The doctor carefully positions the stent so that it covers the narrowed area.
Once the stent is in the correct position, it is released and expands against the airway walls. This expansion immediately creates a wider passage for airflow.
The bronchoscope allows the doctor to confirm that the stent is positioned correctly and that the airway is open.
After the stent is placed, the bronchoscope is removed and the patient is monitored during recovery.
Types of Tracheal Stents
Different types of airway stents may be used depending on the patient’s condition.
Silicone stents are flexible tubes that can be removed or adjusted if necessary. They are commonly used when doctors expect the airway condition to improve over time.
Metal stents are made of expandable mesh that provides strong structural support to the airway. These stents expand once placed inside the airway and are often used in more complex airway obstructions.
The choice of stent depends on factors such as the location of the blockage, the cause of the narrowing, and the expected duration of treatment.
Doctors carefully select the most appropriate stent for each patient.
What Patients Experience After Stent Placement
Many patients notice improvement in breathing soon after the stent is placed. Because the airway is reopened, airflow becomes smoother and breathing feels easier.
Activities that previously caused breathlessness, such as walking or speaking for long periods, often become more comfortable.
Some patients may experience mild coughing or throat irritation shortly after the procedure. These symptoms usually improve within a short time.
Doctors typically monitor patients after the procedure to ensure that breathing remains stable.
Most patients are able to return to normal daily activities within a few days.
Follow-Up Care and Monitoring
Regular follow-up care is important after tracheal stent placement.
Doctors may schedule follow-up visits to check the airway and ensure that the stent remains in the correct position. Imaging tests or repeat bronchoscopy may be used to monitor the airway.
Patients are encouraged to report symptoms such as worsening breathlessness, excessive coughing, or increased mucus production.
Early detection of potential problems helps ensure that the stent continues to function effectively.
The Role of Interventional Pulmonology
Tracheal stent placement is part of a specialized medical field called interventional pulmonology. Interventional pulmonologists are lung specialists trained to perform advanced bronchoscopic procedures.
These specialists use minimally invasive techniques to diagnose and treat airway conditions.
Procedures such as airway dilation, tumor removal, cryotherapy, and stent placement allow doctors to treat complex airway problems without major surgery.
Advances in interventional pulmonology have significantly improved treatment options for patients with airway obstruction.
Conclusion
Severe airway blockage can make breathing difficult and significantly affect quality of life. When conditions such as tracheal stenosis, tumors, or airway collapse restrict airflow, doctors may recommend bronchoscopic tracheal stent placement.
This minimally invasive procedure uses bronchoscopy to place a small support tube inside the airway, helping keep the airway open and allowing air to move freely into the lungs.
With modern bronchoscopic techniques and specialized airway care, many patients experience rapid improvement in breathing and are able to return to normal daily activities.
If you or a loved one are experiencing persistent breathlessness, noisy breathing, or symptoms of airway obstruction, consult a pulmonologist or interventional pulmonology specialist. Early evaluation can determine whether treatments such as bronchoscopic tracheal stent placement may help restore comfortable breathing.
References and Sources
Cleveland Clinic – Airway Stents and Tracheal Stenosis

























