The majority of patients never acquire diabetes because the pancreas's head remains intact and continues to generate insulin. Nonetheless, when the pancreas is not healthy, the odds of developing "Type 3c" diabetes are minimal. During the healing time, the medical staff monitors the blood sugar levels.

Introduction
A Distal Pancreatectomy is a specialised surgical procedure primarily performed to treat tumours located in the body or tail of the pancreas. It may also be used for certain cysts, pancreatic neuroendocrine tumours, trauma, or chronic pancreatitis affecting this part of the pancreas, requiring similar precision to a Sarcoma surgery when addressing complex growths.
Due to the close proximity of the pancreas and major blood vessels, surgical professionals at Gleneagles Hospitals must perform this procedure to achieve clear surgical margins and remove diseased tissue. This article highlights the medical considerations unique to distal pancreatectomy, surgical methods, and the overall recovery process. Such knowledge enables patients to make informed decisions about their course of treatment and to understand the high-quality surgical care provided to maintain their health in the long run.
Understanding the Role of the Pancreas
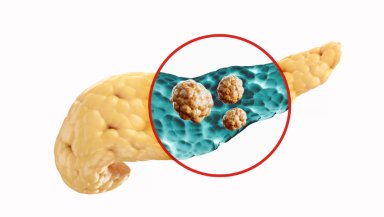
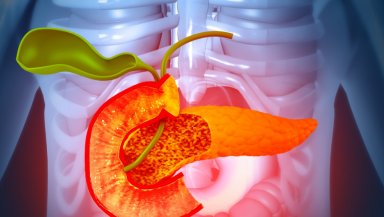
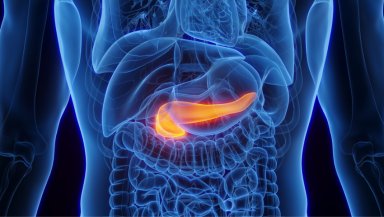
The pancreas is an important gland located deep within the abdomen (just behind the stomach). It has two major roles, i.e., secreting digestive enzymes that help break down food and releasing hormones such as insulin to control blood sugar levels. The organ is separated into three parts: the head (the part placed in a small intestine curve), the body (the middle part), and the tail (the slender part that is directed at the spleen), which can sometimes be accessed via interventional radiology for diagnostic purposes.
Tumours can develop in the body or tail of the pancreas due to primary pancreatic disease, cystic lesions, neuroendocrine tumours, or metastatic deposits. By removing this particular part, the surgeons can leave the remaining pancreas, including the head, continues to retain significant endocrine and exocrine function.
Clinical Indications for Distal Pancreatectomy
Experts at the Gleneagles Hospitals prescribe distal pancreatectomy due to several clinical causes:
- Pancreatic Neuroendocrine Tumours: This usually occurs in the body or the tail of the pancreas.
- Cystic Neoplasms: There are some forms of cysts in the pancreas, which are highly likely to turn into cancer and need to be removed.
- Localised Metastasis: This occurs when liver or other abdominal cancerous cells metastasise to a particular section of the tail of the pancreas.
- Trauma or Chronic Inflammation: Severe injury or localised chronic pancreatitis that affects only the distal portion of the organ.
By removing only the required part, surgeons are trying to balance between the total elimination of the cancer and the sparing of the healthy and functioning tissue.
The Surgical Procedure at Gleneagles Hospitals
Gleneagles Hospitals' surgical unit employs cutting-edge technology to ensure precision and safety during each distal pancreatectomy.
The Role of the Spleen
Since the tail of the pancreas lies adjacent to the spleen and shares its blood vessels, surgeons typically remove the spleen. This is referred to as a distal pancreatectomy and splenectomy. Nevertheless, when the tumour is benign or it is not located in the splenic vessels, there could be a possibility of performing a spleen-preserving distal pancreatectomy.
Surgical Methods
Depending on the condition of the patient and the tumour size, surgeons select the most suitable approach:
- Laparoscopic Surgery: This is a minimally invasive method that uses a few small incisions and a camera. It often leads to less pain and faster recovery.
- Robotic-Assisted Surgery: Robotic technology offers an even higher degree of accuracy and precision, particularly in small areas, and can be especially useful for performing precise dissection near blood vessels or for preserving the spleen.
- Open Surgery: A standard abdominal incision might also be made to access larger tumours or those that may have metastasised to other organs, enabling the surgeon to complete the resection.
Your health matters – get expert advice today.
Recovery and Post-Operative Care
Gleneagles Hospitals prioritises post-operative care, which includes monitoring organ function and managing pain.
- Hospital Stay: Patients are typically in the hospital for three to seven days. The duration varies according to whether the procedure was minimally invasive or open.
- Monitoring Blood Sugar: Because the pancreas produces insulin to regulate blood sugar, health professionals frequently monitor patients' blood sugar levels. Most patients retain enough of the pancreas to maintain normal levels, but some may experience temporary or permanent changes.
- Vaccinations: If the spleen is removed, the care team will ensure the patient receives specific immunisations to protect them from bacterial infections, as the spleen is a vital part of the immune system.
Potential Risks and Safety Measures
Although distal pancreatectomy is usually safe when performed with current surgical methods, the medical team informs patients of the associated risks.
- Pancreatic Leak: The most common specific complication is leakage of digestive fluids from the cut surface of the pancreas. To alleviate this, doctors typically place a temporary drain while the tissue heals.
- Digestion Changes: Certain patients may experience the necessity to take enzyme supplements in case the pancreas does not secrete suitable levels of digestive enzymes.
- Blood Clots: As with any major abdominal surgery, there is a possibility of blood clots. Compression stockings and early movement guidelines are applied to the care team to avoid this.
Why Choose Gleneagles Hospitals?
Gleneagles Hospitals provides a comprehensive approach to difficult hepatobiliary and pancreatic procedures. The hospital provides:
- Experienced Surgeons: Surgeons who carry out a large number of pancreatic and liver resections with good results.
- Integrated Care: This is a team of endocrinologists, dietitians, and oncologists who manage the patient's pre- and post-operative care.
- State-of-the-art Imaging: Surgical guidance is available in real time, and high-resolution diagnostic tools enable the highest accuracy.
- Patient-Centred Support: Patients are supported by specialised nursing staff and physical therapists who provide support with all stages of the recovery process.
Conclusion
A distal pancreatectomy is an important surgical approach for treating tumours in the body and tail of the pancreas, particularly when they are coupled with complicated hepatic or biliary disease. Utilising the most sophisticated minimally invasive techniques, Gleneagles Hospitals ensures that patients receive highly precise treatment, with an emphasis on speedy recovery. Patients will be able to overcome the difficulties of surgery and return to their normal quality of life with support from a diverse team.
Dr Gaurav Singh
Sr Consultant - Surgical Gastroenterologist and Bariatric Surgery
MBBS, MS (Gen Surgery), MCh (Surgical Gastroenterology)
Experience: 16+ Years
General Surgery and Minimal Access Surgery, Surgical Gastroenterology
Bengaluru, KengeriDr Jayanth H
Consultant - Surgical Gastroenterologist & Robotic Surgery
MBBS, MS (Gen Surgery), DrNB (Surgical Gastroenterology), Fellowship (Robotic Surgical Oncology)
Experience: 10+ Years
Surgical Gastroenterology, General Surgery and Minimal Access Surgery
Bengaluru, KengeriDr Adarsh C K
HOD & Sr Consultant - Medical Gastroenterology, Hepatology & Advanced Endoscopy
MBBS, MD (Gen Medicine), DNB (Gastroenterology)
Dr Shailesh Shrikhande
Director & Head - Surgical Oncology
MS,MD,FRCS (England)-Honorary,FRCS (Edinburgh)-Honorary,FACS-Honorary,FASA-Honorary
Frequently Asked Questions
Yes, it is possible to live a healthy life without a pancreas. However, you will need regular insulin injections, proper medical management, and additional measures if you become unwell.
The distal pancreatectomy usually takes between two and four hours, depending on the severity of the case and whether the procedure is performed laparoscopically or open.
Pancreatic secretion of digestive enzymes that leaks from the surgical seal is called a pancreatic leak. The majority of leaks are minor and may resolve on their own with a brief drain operation.
Recovery times vary for different patients. After three to four weeks, individuals recovering from laparoscopic surgery can resume light work. In the case of open surgery, complete recovery and return to normal work might take six to eight weeks.