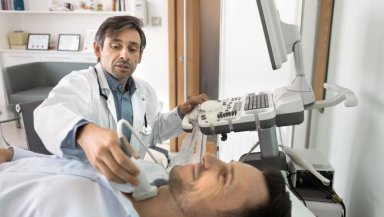
Is I-131 Worth It for Low-Risk Thyroid Cancer? Real Patient Debates and Doctor Insights
Medicine Made Simple
For low-risk thyroid cancer, I-131 therapy is not always necessary. These cancers are usually small, slow-growing, and have a low chance of coming back after surgery. In such cases, doctors may recommend observation instead of additional treatment. However, some patients may still benefit from I-131 depending on specific factors. The decision depends on balancing benefits and risks while considering I-131 safety. Understanding why there is debate around this treatment helps patients make informed choices and feel more confident in their care plan.
Understanding What “Low-Risk” Thyroid Cancer Means
When doctors describe thyroid cancer as low risk, they are referring to tumors that have a very low chance of spreading or coming back after surgery.
These cancers are usually small in size and confined to the thyroid gland. They often grow slowly and respond well to treatment.
Patients in this category generally have an excellent prognosis. Many can live a normal life after surgery without additional treatment.
Because of this, the need for I-131 therapy in low-risk cases is often questioned.
Why I-131 Was Traditionally Given to Most Patients
In the past, I-131 therapy was commonly given to many thyroid cancer patients, including those with low-risk disease.
The idea was to eliminate any remaining thyroid tissue and reduce even the smallest chance of recurrence.
Doctors preferred a more aggressive approach to ensure that no cancer cells were left behind, often standardizing the I-131 treatment process.
However, over time, research showed that many low-risk patients did well without I-131. This led to a change in treatment guidelines.
Why the Debate Exists Today
Today, there is an ongoing discussion about whether I-131 is necessary for low-risk patients.
Some doctors believe that avoiding unnecessary treatment is better, especially when the risk of recurrence is already low.
Others feel that I-131 provides an added layer of safety, even if the benefit is small.
Patients often hear different opinions, which can make the decision confusing, particularly around factors like I-131 dosage.
Understanding both sides of the debate helps patients make a more informed choice.
Arguments for Not Using I-131 in Low-Risk Cases
One of the main reasons to avoid I-131 is that the benefit may be very small in low-risk patients.
Surgery alone is often enough to remove the cancer. Follow-up tests can monitor the patient effectively without additional treatment.
Avoiding I-131 also means avoiding potential side effects, even if they are mild, and reduces the need for I-131 isolation rules.
Many patients prefer to avoid unnecessary treatment when the expected benefit is limited.
This approach focuses on minimizing intervention while maintaining good outcomes.
Arguments for Using I-131 in Some Cases
On the other hand, some doctors recommend I-131 even in certain low-risk cases.
They believe that removing all remaining thyroid tissue can make follow-up easier and more accurate.
In some situations, there may be small factors that slightly increase risk, such as microscopic spread or uncertain findings in reports.
For these patients, I-131 may provide additional reassurance.
The decision often depends on individual details rather than a strict category.
What Research and Guidelines Suggest
Recent guidelines have moved towards a more selective approach.
They suggest that I-131 should not be routinely used for all low-risk patients. Instead, it should be considered only when there are specific reasons.
Studies have shown that survival rates are excellent in low-risk patients, even without I-131.
This has helped reduce the use of unnecessary treatment and focus on personalized care.
Doctors now aim to balance effectiveness with quality of life.
How Doctors Assess Your Individual Case
Even within the low-risk group, not all patients are exactly the same.
Doctors look at several factors before making a recommendation. These include tumor size, margins, lymph node involvement, and pathology findings.
They also consider patient age and overall health.
Based on these details, they decide whether the benefits of I-131 outweigh the risks.
This individualized approach ensures that each patient receives appropriate care.
Patient Concerns and Emotional Factors
For many patients, the decision is not just medical but also emotional.
Some feel more comfortable taking I-131 because it gives them a sense of security. They feel that everything possible has been done to prevent recurrence.
Others prefer to avoid additional treatment and focus on recovery after surgery.
These feelings are valid and should be discussed openly with the medical team.
Understanding both medical facts and personal preferences is important in decision-making.
Pros and Cons in Simple Terms
Choosing whether to take I-131 involves weighing benefits and risks.
The benefit is the potential to remove any remaining cells and reduce recurrence risk further.
The downside is exposure to radiation and possible side effects, even if they are mild.
For low-risk patients, the difference in outcomes may be small. This is why the decision is often optional rather than mandatory.
What Happens If You Choose Observation
Patients who do not take I-131 are closely monitored.
Follow-up includes regular blood tests and imaging when needed.
Doctors track markers such as thyroglobulin levels to detect any changes early.
This approach is safe for many low-risk patients and allows treatment to be given later if needed.
It avoids unnecessary exposure while maintaining careful observation.
Making the Right Decision for You
There is no single correct answer for every patient.
The right decision depends on individual risk, medical advice, and personal comfort.
Patients should take time to understand their condition and ask questions.
Discussing options with the doctor helps clarify the benefits and limitations of each approach.
A confident decision comes from understanding both the science and personal priorities.
Why This Decision Feels Difficult
The decision can feel challenging because it involves choosing between doing more or doing less.
Some patients worry about regret if they skip treatment. Others worry about unnecessary exposure if they take it.
This balance can be difficult to navigate without clear guidance.
Understanding that both options can be valid helps reduce pressure and confusion.
Conclusion
If you or a loved one has been diagnosed with low-risk thyroid cancer, discuss the role of I-131 therapy in detail with your doctor. Ask about your individual risk, expected benefits, and follow-up plan. Taking time to understand your options will help you make a confident and informed decision that aligns with your health and peace of mind.