Why Sarcoma Is Often Misdiagnosed Before Surgery — And How That Affects Outcomes
Medicine Made Simple Summary
Sarcoma is frequently misdiagnosed before surgery because it often looks like a harmless lump and causes little or no pain in the early stages. Many patients are told it is a benign growth and undergo surgery without proper scans or biopsy. This can leave cancer cells behind and increase the risk of recurrence, repeat surgery, or more aggressive treatment later. Understanding why sarcoma is missed and how early decisions affect outcomes helps patients ask the right questions and avoid preventable mistakes.
Introduction
Sarcoma is one of the most commonly misdiagnosed cancers, not because doctors are careless, but because sarcoma does not behave like most cancers. It grows quietly, looks innocent, and often affects people who otherwise feel healthy. By the time it is correctly identified, important decisions may already have been made.
Many sarcoma patients later discover that their first surgery was done under the assumption that the lump was harmless. This realization can be frightening and frustrating. Understanding why this happens is the first step toward protecting yourself or a loved one from avoidable complications.
This article explains, in simple language, why sarcoma is often misdiagnosed before surgery and how those early mistakes can affect long-term outcomes.
Sarcoma Often Looks Like a Harmless Lump
Most people associate cancer with pain, rapid weight loss, or obvious illness. Sarcoma rarely fits this picture early on.
Sarcomas usually appear as slow-growing, painless lumps. They may feel soft or firm and often move slightly under the skin. Because of this, they are commonly mistaken for benign conditions such as lipomas, cysts, or muscle injuries.
When a lump does not hurt and does not cause obvious symptoms, both patients and doctors may assume it is harmless.
Why Being Painless Is Misleading
Pain is often what pushes people to seek urgent medical care. Sarcomas frequently do not cause pain until they become large or press on nerves.
This lack of pain creates a false sense of safety. Patients may wait months or years before seeking evaluation. Even when they do, the absence of pain may lead to reassurance rather than further investigation.
Unfortunately, painless does not mean harmless when it comes to sarcoma.
Sarcoma Is Rare, and That Matters
Sarcoma is a rare cancer. Most general doctors may see only one or two cases in their entire career, if any at all.
Because of this rarity, sarcoma is not always at the top of the list when evaluating a lump. Doctors are trained to think of common conditions first, and most lumps truly are benign.
This statistical reality contributes to delayed or missed diagnosis.
Why Imaging Is Sometimes Skipped
For many small or superficial lumps, imaging may not be ordered immediately. Ultrasound or simple observation is often used.
While this approach is reasonable for many benign conditions, it can be risky for sarcoma. Some sarcomas do not show clear warning signs on basic imaging.
Advanced imaging such as MRI is often needed to understand how a mass behaves within surrounding tissues. Without it, sarcoma may be underestimated, particularly when comparing Soft Tissue vs Bone Sarcoma Surgery planning needs.
The Problem With “Watch and Wait”
Patients are often advised to observe a lump and return if it grows or becomes painful.
In sarcoma, growth may be slow and subtle. Months may pass without obvious change. During this time, the tumor can silently extend into surrounding tissue.
By the time changes become noticeable, the tumor may be larger and more difficult to treat.
Watchful waiting can be dangerous when sarcoma is a possibility.
Why Biopsy Is Sometimes Done Incorrectly
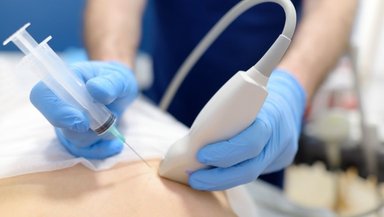
A biopsy is critical for diagnosing sarcoma, but it must be done carefully.
When biopsies are done without proper planning, they can spread cancer cells along the biopsy track. This contaminates surrounding tissue and complicates future surgery.
In some cases, biopsies are done after the lump has already been removed, which eliminates the chance to plan surgery properly.
Incorrect biopsy technique is a common problem in sarcoma care.
The Danger of Unplanned Surgery
One of the most serious consequences of misdiagnosis is unplanned excision. This happens when a lump is surgically removed without knowing it is sarcoma.
Surgeons may remove only the visible mass, assuming it is benign. No margins are taken, and surrounding tissue is left behind, increasing Sarcoma Tumor Removal Risks.
When pathology later reveals sarcoma, the patient often needs repeat surgery, radiation, or more aggressive treatment.
Unplanned excision significantly increases the risk of recurrence.
How Misdiagnosis Changes Surgical Outcomes
The first surgery is the most important surgery in sarcoma. When it is done incorrectly, outcomes suffer.
Cancer cells left behind after unplanned excision can regrow and spread. Repeat surgery may need to be wider and more destructive.
In some cases, limb-sparing surgery that was once possible becomes much harder or impossible.
Misdiagnosis turns a manageable situation into a more complex one.
Why Repeat Surgery Is Common After Misdiagnosis
Many patients are shocked when told they need another surgery after their tumor was already removed.
This happens because the first surgery did not remove the tumor with adequate margins. Repeat surgery is needed to clear remaining cancer cells and achieve Clear Margins in Sarcoma Surgery.
Repeat surgery increases physical and emotional stress and prolongs recovery.
It is often preventable with correct diagnosis from the start.
Impact on Radiation and Chemotherapy Decisions
Misdiagnosis can change the entire treatment plan.
Patients who might have avoided radiation may now need it to reduce recurrence risk. Chemotherapy decisions may also change.
These additional treatments can affect quality of life, fertility, and long-term health.
Early correct diagnosis helps avoid overtreatment.
Why Sarcoma Is Often Diagnosed After Surgery
In many cases, sarcoma is diagnosed only after the lump has been removed and sent for pathology.
While pathology confirms the diagnosis, it comes too late to guide proper surgical planning.
This sequence is backwards for sarcoma care.
Ideally, diagnosis should come before any surgery is done.
How Delayed Diagnosis Affects Survival
Delayed diagnosis and misdiagnosis increase the risk of local recurrence. Recurrence makes sarcoma harder to control.
While not every misdiagnosed case leads to worse survival, the risk is significantly higher.
Early, planned treatment offers the best chance for long-term control.
Why Younger Patients Are Often Affected
Sarcoma often affects children and young adults. This age group is less likely to be suspected of having cancer.
Lumps in young people are often attributed to sports injuries, growth changes, or benign conditions.
This age bias contributes to delayed diagnosis and misdiagnosis.
How Patients Can Advocate for Themselves
Patients who understand sarcoma warning signs can ask better questions.
Lumps that are growing, larger than a few centimeters, deep, or firm deserve proper evaluation.
Asking for imaging and referral to a specialist is reasonable and important.
Self-advocacy can change outcomes.
Why Specialist Evaluation Matters Early
Sarcoma specialists are trained to recognize subtle warning signs.
They understand when imaging, biopsy, and referral are needed.
Early referral reduces the risk of misdiagnosis and unplanned surgery.
Specialist care improves both cancer control and function preservation.
The Emotional Impact of Misdiagnosis
Learning that cancer was missed or mishandled can cause anger, guilt, and loss of trust.
Patients may blame themselves for not pushing harder. This is unfair.
Sarcoma misdiagnosis is a system problem, not a patient failure.
Understanding this helps emotional healing.
Why Awareness Is Improving but Still Limited
Sarcoma awareness has improved, but it remains low compared to other cancers.
Education efforts continue, but rarity remains a challenge.
Patients and families play an important role in spreading awareness.
What Families Should Know
Families often notice lumps before patients do.
Encouraging evaluation and supporting second opinions can make a difference.
Family advocacy matters.
When to Seek a Second Opinion
If a lump is growing, deep, or unexplained, and answers are unclear, seeking a second opinion is wise.
This is not distrust. It is responsible care.
Sarcoma outcomes improve when handled correctly from the start.
What Patients Wish They Had Known Earlier
Many sarcoma patients say they wish they had known that painless lumps can be dangerous.
They wish they had asked more questions before surgery.
Learning from these experiences can help others avoid the same path.
How Knowledge Changes the Journey
Understanding why sarcoma is misdiagnosed helps patients regain a sense of control.
Knowledge transforms fear into action.
Informed patients are better protected.
Conclusion: Early Accuracy Changes Everything
Sarcoma is often misdiagnosed because it looks harmless, grows quietly, and is rare.
These factors lead to delayed diagnosis, unplanned surgery, and more complex treatment.
Understanding these risks empowers patients to seek proper evaluation and specialized care early.
The right diagnosis at the right time can change outcomes dramatically.
If you or a loved one has a lump that is growing, deep, or unexplained, ask whether sarcoma has been considered and whether specialist evaluation is needed. Early clarity can prevent avoidable complications and improve long-term results.
References and Sources
Soft Tissue Sarcoma — National Cancer Institute
Signs and Symptoms of Soft Tissue Sarcoma — American Cancer Society