Why Do Some People Develop Breathing Problems After ICU Intubation?
Medicine Made Simple
Many patients in the intensive care unit (ICU) need help breathing through a tube placed in the windpipe, a procedure called intubation. This treatment saves lives during serious illness. For most people, breathing returns to normal once the tube is removed. However, some patients develop breathing problems weeks or months later. One possible reason is narrowing of the windpipe caused by scar tissue, a condition called post intubation tracheal stenosis. This can lead to breathlessness, noisy breathing, and coughing. Recognizing these symptoms early and seeking medical evaluation helps doctors diagnose the condition and treat it effectively.
Why Intubation Is Sometimes Necessary
When a person becomes critically ill, the lungs may not be able to supply enough oxygen to the body. In such situations, doctors may place the patient on a ventilator, a machine that supports breathing.
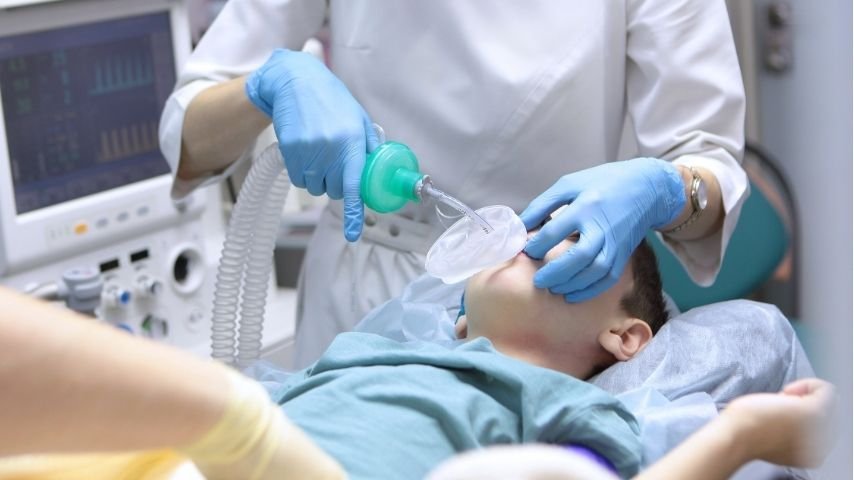
To connect the ventilator to the lungs, a breathing tube is inserted through the mouth and passed into the windpipe. This procedure is called endotracheal intubation.
The breathing tube allows oxygen to reach the lungs and helps remove carbon dioxide from the body. Intubation is commonly used during severe infections, major surgeries, trauma, or conditions that affect the lungs.
Although the idea of a breathing tube can seem alarming, it is an essential and life-saving intervention in many critical situations.
What Happens to the Airway During Intubation
The breathing tube sits inside the trachea, or windpipe, which is the tube that carries air from the throat to the lungs. The trachea is supported by cartilage rings that keep the airway open during breathing.
At the end of the breathing tube, there is a small inflatable cuff. This cuff gently seals the airway so that oxygen delivered by the ventilator goes directly into the lungs instead of escaping.
Doctors carefully monitor the pressure of this cuff to protect the airway. In most cases, the trachea tolerates the breathing tube without any long-term problems.
However, when the tube remains in place for several days or weeks, the pressure and friction from the tube can sometimes affect the lining of the airway.
How the Airway Heals After Intubation
Once the patient recovers from the critical illness, the breathing tube is removed in a process called extubation. After the tube is removed, the airway lining usually heals naturally.
The body repairs the minor irritation caused by the tube, and the airway returns to its normal shape and function.
In some patients, however, the healing process leads to the formation of scar tissue inside the airway. Scar tissue is a natural part of healing, but it is thicker and less flexible than normal tissue.
If scar tissue forms inside the trachea, it may gradually reduce the diameter of the airway. This condition is known as post intubation breathing problems or tracheal stenosis.
What Is Tracheal Stenosis
The word stenosis simply means narrowing. Tracheal stenosis refers to narrowing of the windpipe.
When the airway becomes narrow, it becomes harder for air to move in and out of the lungs. The body must work harder to breathe, which can cause noticeable symptoms.
Even a small reduction in airway diameter can have a significant effect on breathing because airflow resistance increases sharply as the airway becomes narrower.
Tracheal stenosis is one of the most common reasons some patients develop breathing problems after ICU intubation.
When Symptoms Begin to Appear
One of the challenging aspects of tracheal stenosis is that symptoms may not appear immediately after the breathing tube is removed.
Many patients feel completely normal when they leave the hospital. The scar tissue that causes airway narrowing often develops slowly over time.
Symptoms may begin several weeks or even months after the ICU stay. Because of this delay, patients may not immediately connect their breathing problems with their earlier hospitalization.
Common Symptoms After ICU Intubation
Breathing problems caused by airway narrowing often develop gradually.
Shortness of breath is the most common symptom. Patients may first notice difficulty breathing during activities such as walking quickly, climbing stairs, or exercising.
Another symptom is noisy breathing. A high-pitched sound known as stridor causes may occur when air passes through the narrowed airway.
Some patients experience persistent coughing or throat discomfort. Others describe a sensation of tightness in the throat or upper chest.
Because these symptoms resemble asthma or other lung conditions, patients are sometimes treated with inhalers before the true cause is identified.
Why Breathing Problems Are Sometimes Misdiagnosed
When patients develop breathlessness and wheezing-like sounds, doctors may initially suspect asthma or bronchitis. These conditions are far more common than tracheal stenosis.
Asthma medications often help relax the smaller airways inside the lungs. However, if the problem lies in the windpipe rather than the lungs, these medications may not improve symptoms.
When breathing problems persist despite treatment, doctors may begin to investigate other possible causes.
This is when airway narrowing becomes an important possibility to consider.
How Doctors Diagnose Airway Narrowing
Diagnosing tracheal stenosis usually begins with a careful review of the patient’s medical history. Doctors often ask whether the patient recently spent time in the ICU or required ventilator support.
Imaging tests such as a CT scan of the chest help visualize the airway and identify areas of narrowing.
One of the most important diagnostic tools is bronchoscopy. During bronchoscopy, a thin flexible tube with a camera is inserted through the nose or mouth and guided into the airway.
This allows doctors to see the inside of the trachea directly and determine the location and severity of the narrowing.
Bronchoscopy also helps doctors plan the most appropriate treatment.
Treatment Options for Post-Intubation Airway Narrowing
Treatment depends on how severe the airway narrowing is and what caused it.
In many cases, doctors use minimally invasive procedures performed through bronchoscopy.
One common treatment is balloon dilatation. In this procedure, a small balloon is placed inside the narrowed airway and gently inflated to stretch the scar tissue and widen the airway. Patients typically experience smooth tracheal balloon dilatation recovery.
Other bronchoscopic treatments may include laser therapy or cryotherapy to remove abnormal tissue inside the airway.
In some cases, doctors may place a stent inside the airway. A stent is a small tube that helps keep the airway open and allows air to pass more easily.
When the narrowing is severe or involves a long section of the airway, surgery may be recommended. Surgical treatment usually involves removing the scarred portion of the trachea and reconnecting the healthy ends.
Recovery and Long-Term Outlook
With appropriate treatment, many patients experience significant improvement in breathing.
Minimally invasive bronchoscopic procedures often provide rapid relief from symptoms and allow patients to return to normal activities.
However, follow-up care is important because scar tissue may sometimes recur. Regular medical check-ups help ensure that the airway remains open and that symptoms do not return.
Advances in interventional pulmonology have greatly improved treatment outcomes for airway conditions such as tracheal stenosis.
When Patients Should Seek Medical Advice
Patients who experience breathing problems after an ICU stay should not ignore these symptoms.
Persistent breathlessness, noisy breathing, or a whistling sound during breathing should be evaluated by a doctor. Early diagnosis allows doctors to treat airway narrowing before it becomes severe.
Consulting a pulmonologist or airway specialist helps ensure that the correct diagnosis is made and that appropriate treatment is provided.
Conclusion
Intubation is a life-saving procedure used in the ICU to support breathing during serious illness. For most patients, the airway heals normally after the breathing tube is removed.
However, some individuals may develop breathing problems weeks or months later due to scar tissue formation in the windpipe. This condition, known as tracheal stenosis, can narrow the airway and make breathing difficult.
Recognizing symptoms such as breathlessness, noisy breathing, and persistent coughing is important. With modern diagnostic tools and minimally invasive treatments, doctors can successfully restore airflow and improve quality of life for affected patients.
If you or a loved one develop breathing difficulties after an ICU stay or ventilator support, consult a pulmonologist or airway specialist. Early evaluation can identify airway narrowing and help determine the most effective treatment to restore comfortable breathing.

























