Pleural Effusion Explained: Why Fluid Keeps Coming Back and When Thoracoscopy Is Needed
Medicine Made Simple Summary
Pleural effusion means extra fluid collecting around the lungs. In many patients, this fluid can be drained easily. But in some cases, the fluid keeps coming back or does not drain completely. This usually happens when scar tissue forms inside the chest and traps the fluid in pockets or restricts lung expansion. When simple drainage no longer works, doctors may recommend a camera-based procedure called medical thoracoscopy to see inside the chest, remove trapped fluid, and release scar tissue.
Being told you have fluid around your lungs can feel worrying. At first, the solution often sounds simple. Drain the fluid and feel better. Many patients do feel relief after the first drainage. But some are surprised when breathlessness returns and scans show the fluid has come back. They wonder why this keeps happening. They worry something is being missed. They hear new words like loculated effusion, pleural adhesions, or trapped lung. These terms can sound frightening, but the concept is easier than it appears.
Understanding why pleural fluid returns is the first step to understanding why medical thoracoscopy may be needed.
Understanding the Pleural Space
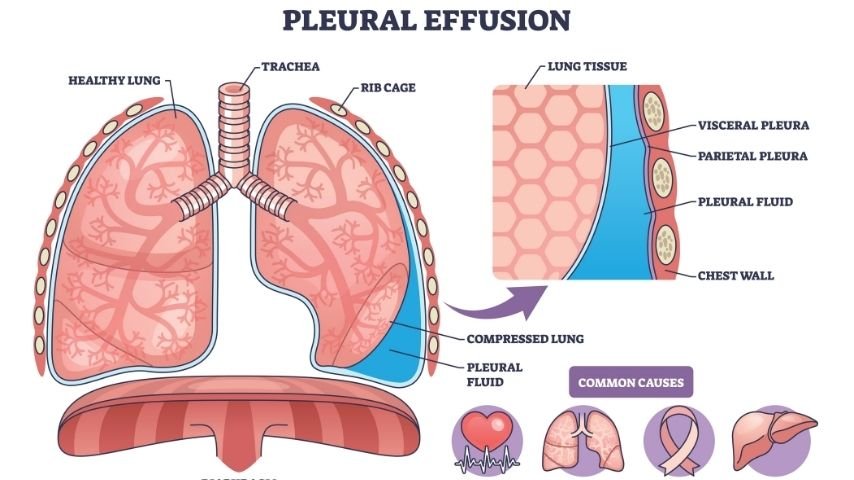
Each lung is covered by a thin lining called the pleura. Another pleural layer lines the inside of the chest wall. Between these two layers is a narrow space containing a small amount of fluid. This fluid allows the lungs to move smoothly while breathing.
When disease affects this space, extra fluid can collect. This is called pleural effusion. The fluid may be caused by infection, tuberculosis, heart problems, liver disease, kidney disease, cancer, or inflammation. The fluid takes up space that the lung normally uses to expand. This is why patients feel breathless.
What Happens When Pleural Effusion Is First Diagnosed
When pleural effusion is found on a chest X-ray or CT scan, doctors usually perform thoracentesis. This means inserting a needle into the pleural space to remove fluid.
This first drainage has two purposes. It relieves breathlessness and it allows the fluid to be tested in the laboratory. These tests often reveal the cause. Many patients improve after this step and do not need further procedures.
But not all pleural effusions behave the same way.
Why Pleural Fluid Sometimes Keeps Coming Back
In some patients, pleural effusion returns even after repeated drainage. There are several reasons this happens.
Sometimes the underlying disease continues to produce fluid. For example, cancer or tuberculosis may keep irritating the pleura. In such cases, treating the main disease becomes essential.
In other patients, the problem is mechanical rather than ongoing fluid production. Inflammation in the pleural space leads to scar tissue formation. This scar tissue creates bands called pleural adhesions. These adhesions divide the pleural space into separate pockets. Fluid gets trapped inside these pockets. Doctors call this loculated pleural effusion. Understanding recurrent pleural effusion causes and treatment helps patients know why this happens.
When fluid is trapped in pockets, a simple needle or chest tube may only drain one pocket. Other pockets remain full. This leads to incomplete drainage and persistent breathlessness.
Over time, adhesions can also restrict lung movement. The lung cannot expand fully even when fluid is drained. This is called trapped lung. In this situation, repeated drainage does not solve the problem because the lung is physically held back by scar tissue.
Signs That Pleural Effusion Is Not Draining Properly
Patients with trapped or loculated pleural effusion often notice that breathlessness returns soon after fluid drainage. Some say they feel only partial relief. Others say they never felt better at all.
Doctors may notice that follow-up scans still show fluid despite a chest tube being placed. Or scans may show unusual shapes of fluid collections rather than one smooth fluid layer.
These clues tell doctors that scar tissue and adhesions are likely present inside the chest. This is why adhesiolysis via medical thoracoscopy may be recommended.
Why Simple Chest Tubes Sometimes Fail
A chest tube is designed to drain fluid that can flow freely in the pleural space. When adhesions divide the space into compartments, the tube cannot reach every pocket. This is like trying to drain water from a room that has internal walls.
Doctors may try repositioning the tube or adding medicines to dissolve partitions. Sometimes this works. But in many cases, the only way to solve the problem is to look directly inside the chest and remove the scar bands.
This is when medical thoracoscopy becomes valuable.
What Medical Thoracoscopy Does Differently
Medical thoracoscopy uses a small camera inserted into the pleural space through a tiny incision between the ribs. This allows doctors to see the pleura, lung surface, fluid pockets, and adhesions directly.
Instead of guessing where the fluid or scar tissue is located, doctors can see it on a screen in real time. They can drain trapped fluid under vision. They can take biopsies from abnormal pleura. They can gently cut adhesions to open fluid pockets and free the lung.
This direct vision is what makes thoracoscopy more effective when simple drainage has failed.
How Thoracoscopy Helps When Fluid Keeps Returning
When thoracoscopy is performed for recurrent pleural effusion, several things happen in one session.
Trapped fluid is completely drained from all pockets. Scar tissue bands are released. This allows the lung to expand more fully. Biopsies are taken to confirm the underlying cause. In some cases, medication is applied to prevent fluid from returning again.
Because both diagnosis and treatment happen together, patients avoid multiple repeated needle drainages and hospital visits.
When Doctors Recommend Thoracoscopy
Doctors consider medical thoracoscopy when pleural effusion keeps returning after repeated thoracentesis. It is also recommended when scans suggest loculated fluid, pleural thickening, or trapped lung.
Another reason is when earlier tests have not identified the cause of the effusion. Thoracoscopy allows precise biopsy under direct vision, increasing diagnostic accuracy.
The decision is based on scan findings, patient symptoms, and previous response to drainage.
What the Procedure Feels Like for Patients
Medical thoracoscopy is usually done under local anesthesia with sedation. The chest wall is numbed. The patient remains relaxed and sleepy.
Most patients feel pressure or mild pulling but not sharp pain. Oxygen and heart rate are monitored throughout. After the procedure, a chest tube is placed to keep the lung expanded.
Patients usually stay in the hospital for one to three days. Mild soreness is common but controlled with medication.
Recovery and Breathing Improvement
Once trapped fluid is removed and adhesions are released, many patients notice improved breathing within days. The lung can expand more freely. Daily activities become easier.
Follow-up scans confirm stable lung expansion. If an underlying disease such as infection or cancer is found, further treatment is started promptly.
For many patients, thoracoscopy marks the turning point from repeated temporary fixes to a long-term solution.
Common Emotional Reactions
Patients often feel frustrated before thoracoscopy because repeated drainage has not solved the problem. They worry that something serious is being missed.
After thoracoscopy, many feel relieved to finally have a clear diagnosis and a mechanical solution to the trapped fluid problem. Understanding what is happening inside the chest reduces fear and uncertainty.
Conclusion
If you or a loved one has pleural effusion that keeps returning or does not drain completely, ask your doctor whether trapped fluid or pleural adhesions may be the reason. Understanding when medical thoracoscopy is needed can prevent repeated procedures and ongoing breathlessness. Book a consultation with an interventional pulmonology or thoracic specialist to discuss advanced pleural treatment options.
References and Sources
American Thoracic Society – Pleural Effusion and Pleural Procedures
British Thoracic Society – Pleural Disease Guidelines
European Respiratory Society – Pleural Space Disorders
Peer-reviewed literature on pleural effusion, adhesions, and thoracoscopy

























