Nurturing Hope Amidst the Storm: The Unseen Challenges of COVID-19

Patients and their families undergo a great deal of suffering when diagnosed with a life-threatening disease such as COVID-19. Unlike other chronic diseases, dealing with COVID-19 patients was different and difficult because the disease was unknown to us and we did not have answers to the patients’ questions. The uncertainty of the disease, the fear of illness and death, the stigma, and socioeconomic hardships all made it even more difficult to deal with the situations in the hospital.
At the end-of-life department, we look after patients with advanced, progressive, incurable or life-limiting diseases so that they can live the final few days with their loved ones and make a few extra memories with their families before they die. The process of care and counselling is not limited to the person who is dying but extends to their families, friends, and caregivers as well. Working at the end-of-life department is quite overwhelming. Watching people lose their loved ones is difficult, and it becomes all the more emotionally challenging when it is a COVID-19 patient as no one is allowed near the patient, they are to be isolated and stay alone.
Suffering from a life-threatening disease and being isolated while fighting the battle alone can take a toll on you emotionally and psychologically. Many times, the patients would scream and yell in agony and fear, would abuse the nurses just to vent out. The disappointed nurses would then come to me and tell me how they did not wish to continue working in the COVID wards. In times as such, I would counsel my team members and tell them how the patient is in pain and struggling for life; there isn’t any grudge against the nurses or the authorities, but the fear of losing their lives and leaving their families alone. It was overwhelming for the nurses in the initial months, but now everybody is well acquainted with the situations and knows how to handle things.
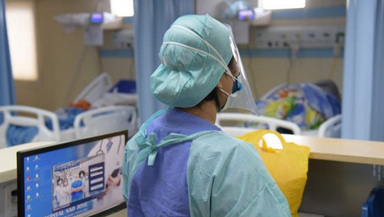
When the pandemic was at its peak and the hospital was full of COVID-19 patients, nurses had to provide care in extreme situations, even in critical care units which were outside the area of their usual practice. None of my nurses backed off from such additional responsibilities. In fact, they spent extra time learning the right ways of doing things to help the patients and their team members, and I am extremely proud of my team.
However, offering clear, accurate and consistent communication to the patients and their families during end-of-life care, in this situation, was challenging. Having access to equipment to provide supportive end-of-life care, was increasingly difficult as demand for supplies increased day-by-day while we approach the height of the pandemic. Creative care planning helped us mitigate some of these challenges along with the determination and diligence of my team.
The initial months, where we had minimal information about the disease, were extremely difficult. We did not have enough PPE kits so we had to use raincoats to protect ourselves. Many of our teammates had contracted the virus and were struggling for life. Doctors had lost hopes with one of them, said she may not recover. This incident was very tough for us to deal with, but thankfully she recovered and has rejoined the team to serve the patients.
One very disturbing challenge that we had to face during the times of the pandemic peak was the process of disposing of the bodies of those who lost their lives. Normally, when a patient died, the family would be informed and they would take their patient home to do the final rites. But during the pandemic, many patients were abandoned by their families, and in such cases, we had to dispose of the bodies with the help of municipal authorities. In such cases, we would dress the body in a fresh hospital gown, wrap it in a blanket, then cover it with a dead-body bag and hand it to the municipal authorities with utmost dignity.
In cases where the families we not allowed near the patients due to the restrictions, we tried to do some of their final rituals because we understand how difficult it must be for the family to not be able to see their loved ones for the one last time. I along with my team made sure that none of our patients or their families feel they are alone in this or that the patients are being discriminated against because they may not survive. The end-of-life care department is dedicated to support and care for patients, and their families, in their final, most vulnerable times.